
© UNICEF Kenya/2021/Lameck Orina.
This story first appeared in The Star newspaper.
It is a brutally hot, dry and dusty day in Garissa town, in the arid region of North-Eastern Kenya, when Kaha Hassan brings her one-year-old son Sudeys to Medina Health Centre. Two consecutive rains have failed in the region and only a few scrubby bushes and skinny animals have survived. Goats with visible ribcages roam the grounds of the health centre, searching for something to eat. The morning sun beats down on the sandy ground, drying it out even more.
Kaha Hassan waits on a bench with six other mothers and young children. When her turn comes, she presents Sudeys to a health worker, who measures his weight and height. Sudeys is calm on the scales but when he has to lie down on the measuring board, he bursts into tears and clings on to his mother afterwards. The health worker writes down his results with satisfaction – his arm measurement has changed from red (severe wasting) to yellow (moderate wasting). She informs Kaha that Sudeys is improving but still malnourished and gives her some ready-to-use therapeutic food to continue his treatment at home.
Kaha and her family were forced to leave their home in Modogashe, 150 km north of Garissa town, where they used to herd animals, due to the drought. “We lost eight of cattle to drought and four goats,” Kaha says in Somali. “We had no pasture, no milk and no water. We couldn’t pay rent anymore.”
Pastoralists have a strong connection to their animals and watching them die was heartbreaking for Kaha’s family. In the end, they felt that they had no choice. Leaving their remaining animals with a relative, they moved to Garissa town to live with Kaha’s mother in law. But then things got even worse.
“Sudeys became weak because I had no milk or food to give him,” Kaha recalls. “At first, I thought he was sick, but he did not recover. When the community health volunteer visited us, he was not moving. He measured my son’s arm and found he had severe acute malnutrition. He told me to take Sudeys to the health centre. As a mother, I was very worried because I didn’t have anything to give him.”
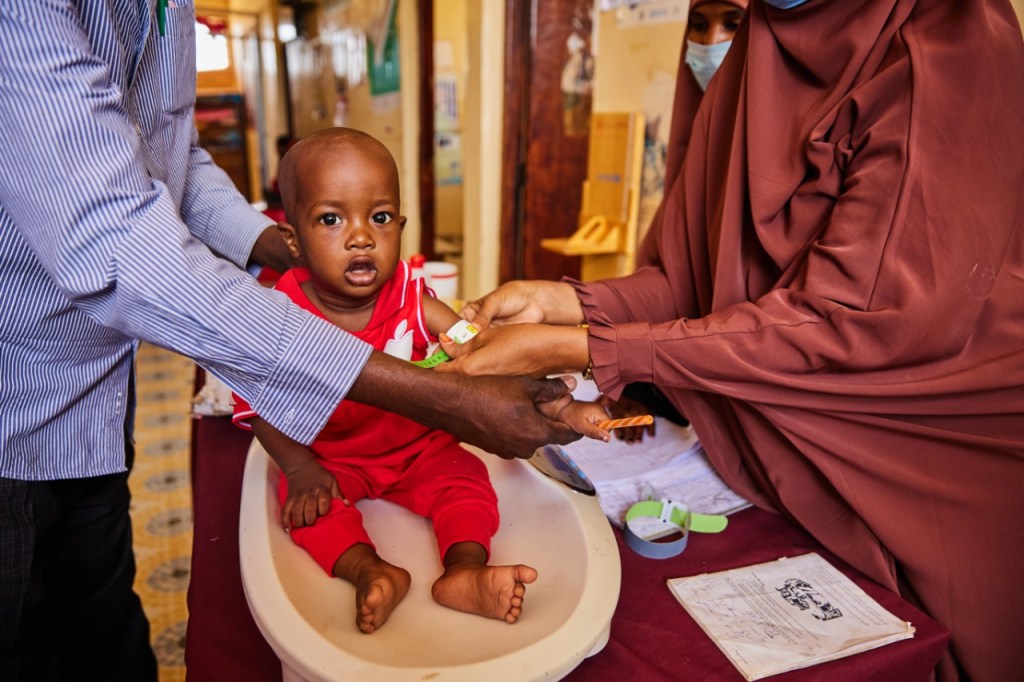
© UNICEF Kenya/2021/Lameck Orina
Prepare and respond
Garissa County is experiencing a prolonged drought, following the failure of two rainy seasons. As an arid and semi-arid land (ASAL) county, droughts in Garissa exacerbate already difficult conditions. Coming on top of the economic impact of the COVID-19 pandemic, the drought has pushed many families like Kaha’s over the edge into poverty. As pastoralists move to towns, the cost of living and burden on urban families also increases.
“In Garissa County, the drought has impacted us so much that we are in crisis,” County Nutrition Coordinator Shamat Yusuf says. “The water pans have all dried up, so the drought is real. Many people are migrating from their previous villages to the town and so many children have been affected. For every 100 children, 17 are acutely malnourished. If it doesn’t rain soon, this is going to worsen.”
UNICEF has supported the national Government to develop an action plan to prevent and treat malnourished children and women in 10 counties that recorded high levels of malnutrition, including Garissa. This action plan covers different sectors that are important in tackling the root causes of malnutrition, such as food security, health, social protection for poor households, water and sanitation.
In Garissa, UNICEF is supporting the county Government, health centres and communities to prepare for and respond to drought. This includes support for health centres with nutrition supplies such as ready-to-use therapeutic food (RUTF), training on integrated management of malnutrition (IMAM), and support for communities with mid-upper arm circumference (MUAC) measurement.
“Young children are the most vulnerable to malnutrition,” UNICEF Nutrition Officer Nicholas Kirimi explains. “We have a tape we use to measure the mid-upper arm circumference of children under five. This helps us identify children who have severe or moderate acute malnutrition, as well as children who are growing healthily.”
He continues: “The measurement is usually done by health care workers and community health volunteers. We have recently started training mothers and caregivers on how to use a ‘family MUAC’ tape, so they can monitor their own children and refer them to the health centre early if they are malnourished.”

© UNICEF Kenya/2021/Lameck Orina
Centre of excellence
At Medina Health Centre, Nutrition Officer Aisha Mohamed points to an integrated management of acute malnutrition (IMAM) chart on the wall. This shows the number of moderate and severe acute malnutrition cases per month, measured against the average monthly cases and rainfall. With red and black marker pens in her hand, she draws two new lines on the chart to indicate the latest monthly cases. The predominant weather is indicated with a small drawing – for all but one month of the year, it is full sun with no rain.
“IMAM acts as a surveillance tool for us at the health facility and in the community to know whenever there is an increase or decrease in malnutrition caseloads,” Aisha explains. “We set thresholds for normal, alert, alarm and emergency. We are now at alarm level. When this happens, we open our malnutrition services daily. We do daily screening at the health centre and in communities, distribute supplies and admit new cases.”
Back at home, Kaha sits on a mattress in the one-room house the family is sharing. Their few possessions are packed into a single suitcase and chest of drawers. Kaha opens a new packet of ready-to-use therapeutic food and gives three quarters of it to Sudeys, while his older brother, two-year-old Khalid, looks on.
Thanks to the help from UNICEF and Medina Health Centre, Sudeys is well on his way to recovery. His behaviour has also begun to return to normal. “I feel happy when I go to the health centre because they are supporting us,” Kaha says. “Sudeys is doing much better now and is even trying to stand. When the drought ends, I hope to go back home and continue to raise my family.”

© UNICEF Kenya/2021/Lameck Orina