
© UNICEF Kenya/2022/Lameck Orina
This story first appeared in The Star newspaper.
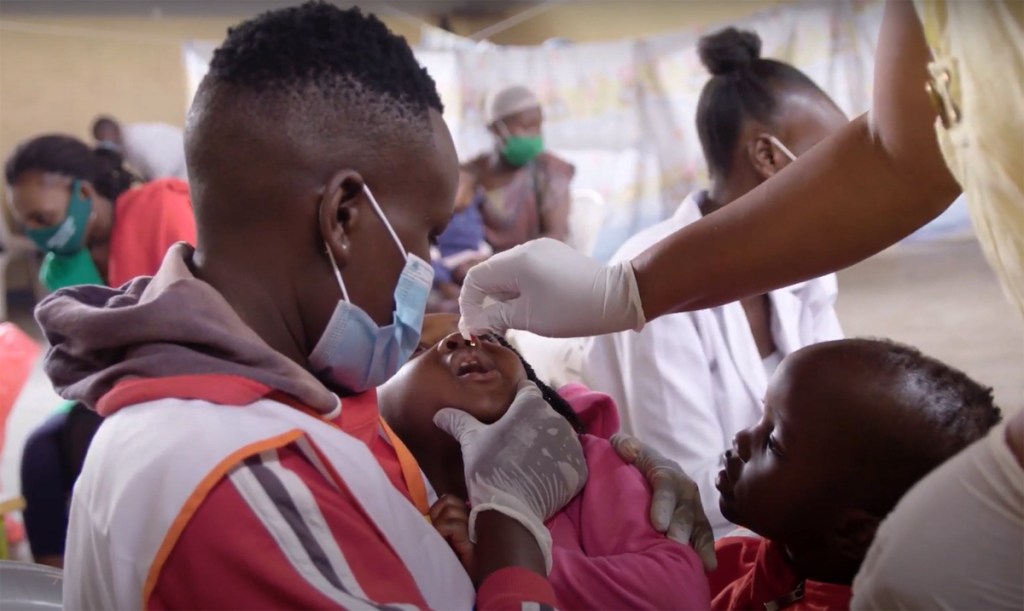
It’s a quiet mid-morning at Bunde Health Centre in Kisumu, when local farmer Alice Mwajuma brings her two children David, 5, and Dahzur, 2, for a check-up. Long antlered cattle wander down the earth road outside, stopping to munch on the occasional patch of green grass. Alice and her boys arrive on a boda-boda motorbike, stopping by a fruit stall on the road outside. The health centre is quiet and cool in the shade of large trees. Blue and white buildings sport graffiti art illustrating health messages, such as the six ante-natal care steps for pregnant women to take.
Alice, David and Dahzur put on masks and wash their hands at a handwashing station at the entrance of the compound, before joining a short queue of mothers and children waiting for their consultations. The two boys have recently developed an itchy red rash on their arms, which Alice is concerned is not going away.
After just a ten-minute wait, the boys are weighed and measured by a nurse. They go with Alice into the consultation room to see a doctor. Then, they are taken to another room for a lab test, back to see the doctor for a diagnosis, and finally to the pharmacy to pick up their medication. The process is quick and efficient, taking less than half an hour.
“The doctor told me that David and Dahzur have a fungal infection,” Alice says afterwards. “She gave me some medicine to treat it. They need to take it for five days and then they should be better. I like coming to the health centre because it’s close by and convenient. We were seen very quickly, and it was not expensive. It is much better than travelling to the district hospital.”

© UNICEF Kenya/Lameck Orina/2022
Universal health care
Primary health care and community health are essential health care made accessible to all families at a cost that they can afford, without incurring catastrophic out of pocket health expenses – which can be a major issue for poor families without health insurance when they go to hospital. By contrast, primary and community health delivers better outcomes for children more efficiently and at a lower cost.
A Ministry of Health investment case has demonstrated that for every US $1 invested in community health, Kenya will reap the equivalent of US $9.4 in economic and social benefits – a return on investment close to ten to one. However, the current coverage of community health services in Kenya is just 59 percent, with some counties as low as 17 percent.
“Primary and community health services are the cornerstones of universal health coverage,” UNICEF’s Chief of Health Yaron Wolman says. “They help prevent ill health and deliver better care for children at a lower cost, meeting up to 90 percent of a child’s health needs. That’s why UNICEF is advocating for an expansion for primary health care and community health services so that all children and families can readily access basic health care at a cost they can afford.”
This is exactly what is happening in Kisumu, where UNICEF has supported the establishment of a Primary Care Network in Nyando Sub-County. This network is piloting an approach based on disease prevention and health promotion at the community level, rather than only on curing disease.
“In this area, 60 percent of child mortality is due to three diseases: malaria, diarrhoea and pneumonia,” Nyando Medical Officer Dr Johnathan Billis explains. “All three can be dealt with most effectively at the primary and community level. For example, we can prevent malaria by distributing bed nets and teaching communities about their importance and proper use. With support from UNICEF, we have trained community health volunteers to identify fever and do rapid tests for malaria, allowing them to diagnose and treat the disease early.”
Care in the community
In nearby Oketha village, Community Health Volunteer (CHV) Faith Achieng pays a visit to Tabitha Achieng, 27, a hairdresser and mother of five children. Inside the family’s small, green-painted house is a comfortable lounge with sofas, a TV and toy panda. There is an alphabet chart on the wall. Faith begins by examining Hazel, 3, who has a cough. She checks his temperature with a thermometer and measures his upper-arm circumference to check for malnutrition. As she works, she fills out the information to send to the local health centre via an app on her mobile phone.

© UNICEF Kenya/Lameck Orina/2022
Faith can find nothing wrong with Hazel apart from the cough, so she advises Tabitha to give him warm water with honey and monitor him until her next visit.
“I’ve visited this family every month for five years,” Faith says. “The children have had malaria and diarrhoea several times. I check the hygiene situation of their toilet and make sure that they treat their water before drinking it. There are a lot of mosquitos in this area, so I also check that they are using bed nets for all the children. When I visited last month, I found that Hazel had malaria. I gave his mother some medicine and he got better in a few days.”
Before she leaves, Faith checks the mosquito nets in the bedroom and shows Tabitha how to hang them properly so that there are no gaps. She promises to return in two days to check up on Hazel.
Thanks to Kisumu County’s focus on primary and community health care, Alice and Tabitha were able to get early treatment for their children, avoiding their conditions becoming much worse and more expensive to treat. However, these services are not yet available to all families in Kenya, which is why UNICEF is advocating for this to be a priority for the next Government.
“We are calling for the next Government on Kenya to increase budgets for primary health care and community health,” UNICEF’s Yaron Wolman says. “We also want them to support community health volunteers with recognition, training and financial incentives. As we have seen in Kisumu, this can substantially improve children’s health.”
Tabitha agrees: “I’m glad that Faith comes to visit us and brings medicine for my children,” she says. “Before we used to have to go to the district hospital and we couldn’t get enough medicine. Now it is much easier. I’m very happy.”
© UNICEF Kenya/2021
One thought on “In Kisumu, healthcare moves closer to communities”